Obesity is managed by conservative (diet and exercise), medical and surgical approaches.
The decision of which treatment is best for you depends on factors such as your BMI, waist circumference and also the presence of other medical problems. Usually combinations of the various approaches are used, directed by guidelines such as the NICE guidelines for NHS patients, although the clinicians overall judgment presides. All studies that directly compare surgical with conservative treatments conclude that surgery is superior in providing long term, sustained weight loss.
The focus of this website is the surgical treatment for obesity.
Is Surgery Suitable?
The National Institute for Health and Clinical Excellence (NICE) have produced guidelines on obesity. It stated that those who have a BMI over 40 or a BMI over 35 accompanied by an existing condition which would benefit from weight loss, are suitable for surgery. Ideally you would have tried to lose weight by diet and exercise and can demonstrate to your surgeon that you will be able to persevere with such measures after the surgery. Obesity management is a lifelong process and not a quick fix. It involves preparation for the surgical procedure and also continual cooperation after the surgery to accompany the weight loss process.

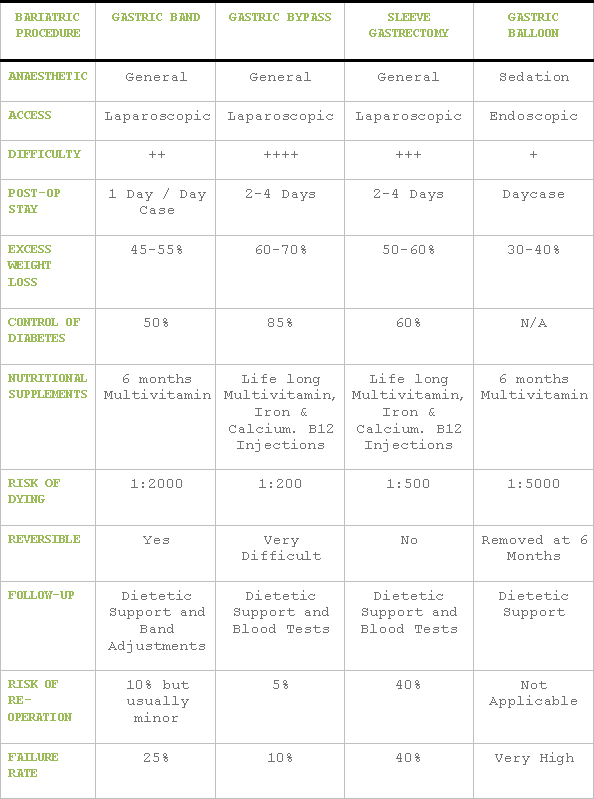
What is Bariatric (Obesity) Surgery
Laparoscopic Gastric Bypass
Laparoscopic Sleeve Gastrectomy
Laparoscopic Gastric Band Insertion
Intra-Gastric Balloon Insertion
Tips for successful weight loss
- Eat three regular meals a day
- Drink fluids between, not with meals
- Stick to textured foods. If you don’t need a knife and fork to eat it, you shouldn’t be having it
- Avoid overeating. If you feel uncomfortable after a meal, you have probably eaten too much too quickly
- Sit at a table to eat, without distractions such as television
- Eat for 20 minutes then stop. You don’t need what you haven’t eaten
- Enjoy leaving food on your plate
- Attend for regular follow-up, including nurse and dietetic appointments
- Join a patient support group
- Plan 20 minutes of aerobic exercise 5 times per week. Exercise to a level where you are out of breath, but can still talk in sentences
- Contact your local bariatric team should you develop any problems or concerns
- Contact your local bariatric team should your weight loss halt at any time. Do not feel a failure, it is important that we know so that we can help
- The above points are helpful for long-term success with all types of weight loss surgery. If you are not able to make this commitment, then weight loss surgery may not be right for you.
Expected Weight Loss
It is important to be realistic about the amount of weight you expect to lose following surgery. Patients lose an average of half (50%) of their excess weight after bariatric surgery. If for example you currently weigh 20 stone and your ideal weight is 10 stone, then you may achieve a five stone weight loss. This is an average, some people will lose a lot more than this but some people will lose less. The average initial weight loss after gastric bypass or sleeve gastrectomy is up to 70% of your excess weight (Up to seven stone in the example above). This weight loss is expected over the first nine months after surgery. If you learn to work with a gastric band, there is no reason why you cannot lose as much weight with band surgery as you would with a gastric bypass, but the weight loss will be slow and gradual over two to three years. There is, however, no guarantee that you will lose this amount of weight, particularly with a gastric band. The advantage over dieting alone is that there is a greater chance that the weight will stay off. Unless you are able to maintain a healthy lifestyle, there is a risk of weight regain, particularly after 3-4 years. The degree of weight loss may not seem huge but is enough to produce significant long-term health benefits.
Keys to success following weight loss surgery include:
- Following the appropriate changes to your eating habits that have been advised
- Relearning the feeling of satisfaction after eating and knowing when to stop
- Instead of seeing how much you can eat, try to see how little you can eat to remove hunger
- As well as controlling diet it is important to increase activity levels. Regular daily activity is best
- Joining a local patient support group and keeping up with the follow-ups that are scheduled with your local bariatric team will all build toward long-term success
- If you have difficulties after weight loss surgery, it is important not to give up and do not feel a failure. Often a brief adjustment to a gastric band or lifestyle can bring you back on track.
Making A Decision
Pre Operative Preparation
Patients who are having Laparoscopic Bariatric (Weight Loss) Surgery will be asked to make appropriate changes to their diet and activity levels to have the greatest chance of success. It is important that patients get in to a habit of eating three regular meals a day, avoid snacks and avoid drinking while eating. We ask that patients continue regular exercise of at least 20 minutes, five times a week. It is better to choose exercise that you enjoy and that can be fitted in to your daily routine. We also recommend that all patients attend a local support group to meet patients that have had the type of surgery that is being considered.
Patients who are able to make the above changes are more likely to have a successful long-term result from Laparoscopic Weight Loss Surgery.
Patients will be asked to attend for a pre-operative assessment to ensure that the operation will be as safe as possible. This can sometimes identify medical problems that you may not have been previously aware of. If patients have a history of stomach problems, particularly acid reflux, they may be asked to have a gastroscopy examination as part of the pre-operative assessment. This will be booked as a separate appointment.
We ask our patients to have a strict two-week diet prior to surgery. A very low calorie diet is prescribed for this period, with the aim to reduce the size of the liver. This is often called the 'Liver Shrinking Diet'. We expect patients to lose an average of 5kg over this period, which is a sign that the diet has been adhered to. The liver is immediately above the top part of the stomach involved in most Laparoscopic Weight Loss Surgery. There is a risk of damage to the liver if it has not reduced in size. This can lead to complications that may result in the procedure being abandoned. Patients are normally weighed on the day of surgery to ensure they have completed the diet. If your weight has not reduced, the procedure may then have to be cancelled.
The Operation - Day of Surgery
The procedure will be carried out under a general anaesthetic (except for a Gastric Balloon), which means you will be asleep throughout. The operation will take between 1-2 hrs although you may be away from your room longer than this as you will spend some time in the theatre recovery area following your surgery.
Feelings of sickness are not uncommon after surgery. It is important that you inform the nurse looking after you at an early stage as prolonged vomiting can pull on the internal stitches. Anti-sickness medication can be given which will rapidly ease any feeling of sickness. Pain relief is given in the early post-operative period. Some patients experience pain from trapped wind during this time that is not completely controlled with pain relief medication. Common symptoms include pain behind the breast bone or into the left shoulder. It is important that you inform your nurse as symptoms can be relieved with simple remedies such as peppermint water or getting up and moving about. Most patients experience minimal pain after the first day.
Most patients will be on an ‘Enhanced Recovery’ pathway post-operatively. Part of this pathway involves a structured process of getting out of bed, regular breathing exercises and early reintroduction of drinks. This combination aids recovery and reduces the risk of complications. It is important that you follow the advice given.
Patients are normally able to go home within 24 hours of a Laparoscopic Gastric Band procedure. Patients usually go home between one and two days after Laparoscopic Gastric Bypass or Laparoscopic Sleeve Gastrectomy surgery.
The bariatric team will be in regular contact to ensure that you continue to make good progress over the early post-operative period. If you experience any problems at all while at home, it is important that you speak to a member of the bariatric team straight away for support and advice. If you feel unwell in the first few days, it is often better to return directly to the hospital where you had your surgery, as they will be in the best position to manage any problems.